Why Radiation Protection Is Important?
Radiation describes a process where energy emitted by certain body travels over the medium and through space, to get absorbed by a different body. Radiation is classified as per the effects that it produces on various matters, in ionizing & non-ionizing radiations. The ionizing radiation includes X rays, cosmic rays, and radiation from the radioactive materials. The non-ionizing radiation are radiant heat, microwaves, radio waves, infrared light, terahertz radiation, ultraviolet light and visible light.
The primary purpose of UTPR is providing right level of safeguard for humans without limiting beneficial actions offering rise to the radiation exposure. The radiation protection is preventing occurrence of the harmful deterministic effects as well as decrease possibility of occurrence of the stochastic effects (like cancer & hereditary effects).
What Is Radiation Protection Important in Radiology
Radiology makes use of techniques like X-ray imaging that will help to detect and diagnose various injuries and diseases, manage proper care of patient, and guide different types of the medical treatment.
As X-rays mainly engage ionizing radiation that will deposit energy in the human cells as well as cause tissue changes, this is quite important to reduce associated risk to any patient. It can be done by limiting radiation exposure to minimum needed to create clinical images required to answer medical question.
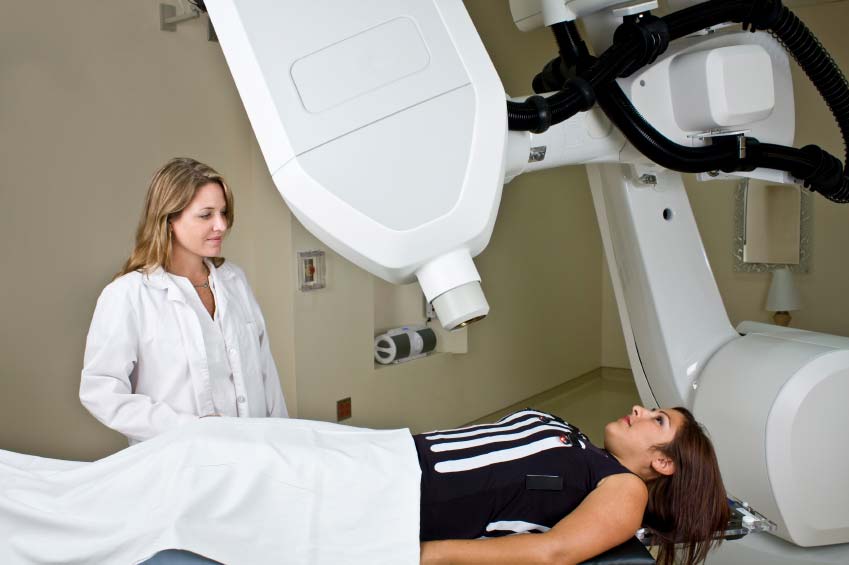
Why’s Radiation Safety A Major Issue?
The root issues of the excessive radiation exposure come from a fact that in a healthcare field people who work under radiation have received just rudimentary radiation training. While interventional radiologists are perfectly trained in safe use of the radiation, vascular surgeons and interventional cardiologists, for example, get minimal radiation training. As they generally are not familiar with the sources of the radiation exposure, they might know much about the risk-reduction or safety strategies.
Compounding this problem is, whereas radiologist’s key member is the radiologic technologist (that has got the radiation safety training), interventional cardiologist and vascular surgeon’s team member can be the nurse, who has received very little or no radiation training. That does not mean that all radiologists use top radiation safety practices. Despite the training, most of them have actually become quite complacent.
Based on various sources, it’s complete safe to say it is one major problem, as public health itself will play a very important role in the radiation safety. This is quite important to point, that efficiency and safety of using this source of the ionizing radiation is a primary component of the Good Medical Practice.